Have you noticed that things are a little different down there? While it’s common to hear about hot flushes and sleepless nights, people tend to keep schtum about other, more personal changes that happen with menopause.
While it’s not the kind of thing you might discuss at the water cooler, vaginal changes affect most women during and after menopause. About half report vaginal tightness, dryness, pain and uncomfortable sex among other problems.
Read on for all the info you won’t get from a group chat.
Find what you need quickly
Hormones and your vagina
At the time of menopause, your ovaries stop producing oestrogen. While this affects many different parts of the body, the dramatic reduction in hormone levels can be particularly troublesome when it comes to the tissues in and around your vagina.
This is because these tissues are rich in oestrogen receptors. During premenopausal life the presence of oestrogen keeps these tissues plump, resilient and healthy. Once oestrogen is removed, you begin to notice changes that can be annoying and in some cases quite distressing. Tissues become thin, sore and, in some cases, inflamed – this condition is called vaginitis.
These changes can also be referred to as:
- Vaginal atrophy
- Atrophic vaginitis
- Vulvovaginal atrophy
- Genitourinary syndrome of menopause (GSM)
In this article we will use the most recent term, GSM, although these terms are often used more or less interchangeably.
Read Cathy’s story and how she found relief from vulval pain.
What genital symptoms should you look out for?
Tissues sensitive to oestrogen are found in your vagina, around the external genitals and in the urethra and bladder. As you would expect, this means that there is a wide range of symptoms caused by hormone changes around menopause.
Genital symptoms can affect the vagina and the external genitalia, including:
- Burning
- Itching
- Pain
- Dryness, which happens due to decreased secretions
- Discharge (usually white or watery)
- Painful sex
- Bleeding, including bleeding after sex
- Recurrent infections
- Pain on sitting down or wiping
You may also notice urinary symptoms, including recurrent urinary tract infections, pain on peeing, blood in your pee and needing to pee more often.
Find out more about urinary symptoms in menopause.
Let’s take a closer look at some of the most common vaginal symptoms…
Burning, itching and pain
You may experience burning, itching and pain either internally or externally. This can be extremely uncomfortable and disruptive, and is one of the most common symptoms of GSM. In some cases it can even be severe enough to disrupt normal activities, including cycling and sitting down.
This happens when typical menopausal changes to the genitals are accompanied by inflammation. The same process can also cause bleeding and changes to the appearance.
Painful sex
Several of the changes seen in menopause can contribute to painful sex. As the effect of oestrogen wanes, the vaginal walls become thinner and more delicate, with a loss of the folds and elasticity which would previously have allowed the vagina to stretch during sex. Add to this reduced natural lubrication and a tendency for the vagina to become narrower and shorter, and you have a recipe for painful sex.
You may also find sex less pleasurable. This happens because blood flow to the area is reduced and because the nerves supplying the genital area also work more effectively in the presence of oestrogen (which is now in decline).”
There are several things you can do to make things more comfortable. Use a water-based lubricant and try to have sex regularly (as this can help maintain the vaginal tissues). Pelvic floor exercises can also help, as they stimulate blood flow to the area and encourage lubrication as well as keeping the pelvic floor muscles in shape.
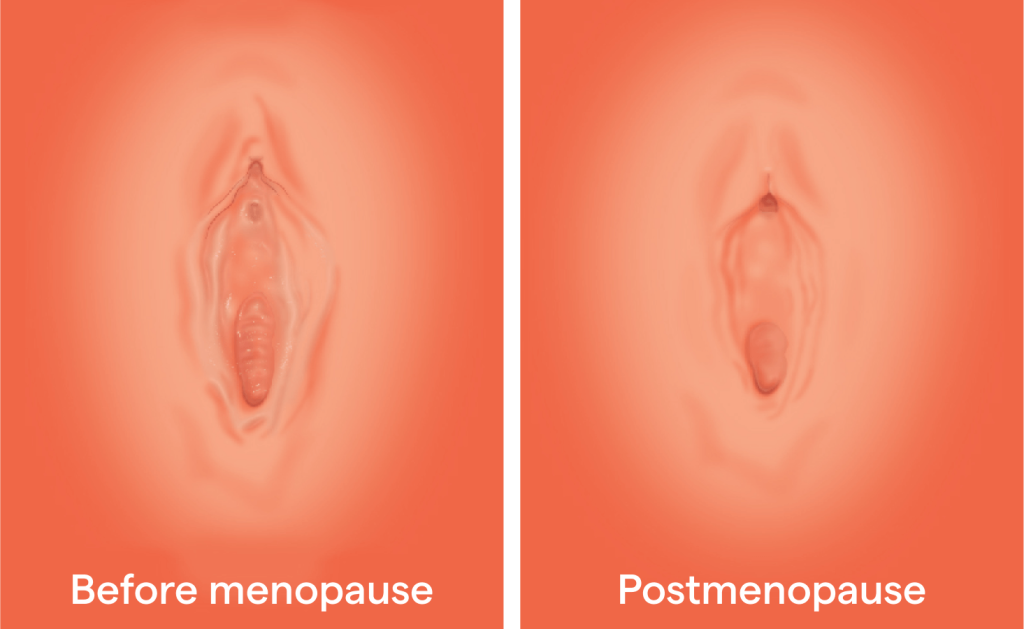
Changes in appearance
You may also notice that you look different down there after going through menopause. This is normal and just like the other symptoms of GSM is due to reduced oestrogen levels – blood flow to the area decreases, collagen and elastin levels drop.
Tissues including the vulva, labia and clitoral hood can all be affected. You may notice that you have less pubic hair, that your labia seem to shrink or even disappear. Some women may find that the labia fuse together, and that the vaginal opening narrows. Internally, the vaginal walls often become paler, drier and smooth in texture.
Prolapse also becomes more common around this time. Speak to your doctor if you notice any fleshy lumps in or protruding from the vaginal opening, especially if they are associated with discomfort, changes to your bowels or bladder, or a dragging sensation.
Read more about prolapse in our menopause symptoms library.
When do changes to your vagina happen?
It varies. Some women will begin to notice changes to their vagina and genitals happening alongside the first symptoms of menopause. Others may only begin to notice problems several years after their other menopause symptoms have disappeared.
When should I see a doctor?
If you have any symptoms that are bothering you, including any from the list above, book an appointment! While this is not an easy subject to talk about, your doctor will have dealt with this problem many times over and can offer effective treatments.
It is important to note that some symptoms of GSM can be caused by other conditions, therefore it’s important to get them assessed properly by your doctor. Book in as soon as possible if you have any vaginal bleeding, blood in your pee, sores or ulcers on the genitals, severe pain or anything that is particularly worrying you.
Are there treatments that work?
HRT
The most effective treatment is hormone replacement therapy (HRT). This involves taking oestrogen supplements, which allow the tissues to heal thanks to those oestrogen receptors mentioned earlier. It usually takes a few months to see their full effect, but most women will eventually notice a significant improvement in their symptoms (including changes to the appearance).
Topical HRT
Unlike most menopausal symptoms, GSM can be treated effectively with topical HRT. This means that the oestrogen is applied directly to the vaginal and/or genital tissues in the form of a cream, ring or pessary (internal tablet).
Read more about HRT risks and benefits.
While other forms of HRT come with warnings about side effects, the risk with topical HRT is extremely low. This is because the type of oestrogen used is both much less potent than that used in other forms of HRT, and not absorbed into the bloodstream. Topical HRT is therefore safe for most women, although you should always check with your doctor before starting treatment (especially if you have a history of breast cancer).
The amount of HRT that you need will also vary. It is normal to begin by applying the product each day for two weeks followed by a gradual reduction in frequency. Once recovered, many women will be able to wean this down to a couple of times per week or even less.
Systemic HRT
Systemic HRT (usually in the form of a tablet or patch) may also help with your symptoms of GSM, although it is not usually given for GSM alone. Some women on systemic HRT may also need topical HRT to fully treat their genital symptoms. Speak to your doctor to find out which option is best for you.
Hygiene
It is also important to pay attention to hygiene and skincare (yes, even down there) as the skin becomes more delicate and prone to inflammation and infection after menopause. Try using a soap substitute to cleanse. Options include aqueous cream or Epaderm, both of which can be bought at your local pharmacy.
Wear cotton knickers and looser clothes, and avoid using sanitary towels and pantyliners where possible. Speak to your doctor if you are having trouble with leaking pee, as this can also contribute to inflammation in the vulval area.
Vaginal moisturisers
Vaginal moisturisers may also help, especially if you are struggling with dryness. These can be purchased at a local pharmacy and common brand names include Replens and Vagisil. Be sure to follow the product instructions carefully and if you are planning to use an internal moisturiser ensure that the product you buy is appropriate for this. Be aware that there is a difference between vagina moisturisers (which help to treat dryness at any time) and lubricants (which are specifically used to make sex more comfortable).
Probiotics
The vagina is colonised and kept healthy by a variety of different species of fungi, viruses and bacteria, mainly Lactobacillus. During menopause, these bacteria are thought to affect a number of vaginal symptoms, such as pain, dryness, loss of lubrication, and painful sex. There are lots of different species of Lactobacillus, although the most common in healthy vaginas include Lactobacillus iners and Lactobacillus crispatus.
Supplementing with vaginal and oral probiotics containing strains of Lactobacillus may support the vaginal microbiome and increase bacterial diversity in the gut. Indeed, small studies have shown that, if taken orally, these may affect vaginal health and reduce vaginal infections. Although initial findings are encouraging, more research is needed in this area.
Physio
If you do not find much improvement, it may also be worth considering attending physio for assessment of your pelvic floor. Your doctor will be able to advise whether this is necessary.
Final word
However these changes affect you, remember that effective and safe treatments are available. You don’t have to put up with it if you don’t want to! Your doctor will be able to discuss the best treatment options for you.
Read more about menopause on our blog and learn more about UTIs in our symptoms library.